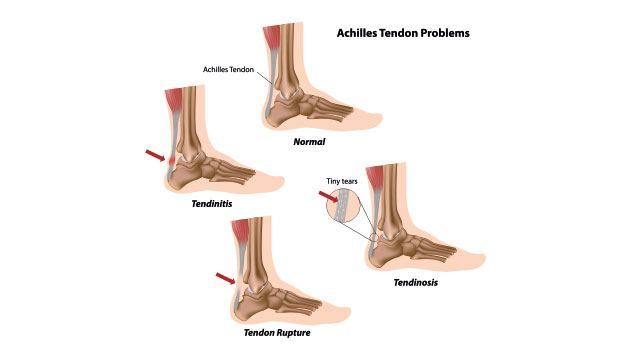
The Achilles tendon is a band of tissue that connects the calf muscles to the heel. The Achilles tendon is the thickest and strongest tendon in the body; a healthy Achilles tendon is capable of taking up to 2 tonnes of load through it. Contracting the calf muscles pulls the Achilles tendon, which causes the foot to move downwards and the heel to raise – an action that is part of walking, running, jumping, landing and standing on the toes.
Achilles Tendinopathy
Achilles tendinopathy is the most common cause of Achilles pain. It tends to come on gradually and is associated with a degeneration of the tendon, causing pain and sometimes thickening in the tendon. It is important for your physiotherapist to establish which part of the tendon is causing your problem as this will affect the type of treatment you require.
Treatment usually begins with an eccentric loading program and may progress to involve stretches, strengthening exercises, assessment of footwear and foot position, and advice regarding your sporting activities. Although this can be a stubborn and sometimes frustrating condition, it will normally resolve with physiotherapy.
Achilles Rupture/Tears
A rupture of the Achilles tendon is a partial or complete tear of the tendon. It occurs suddenly, sometimes with a popping sound, and is normally very debilitating. Some people describe rupturing the Achilles tendon as feeling like they have been shot in the back of the ankle.
A full rupture means the Achilles tendon is completely torn so that it no longer connects the calf muscle to the heel which means the calf muscle is completely unable to function. Achilles tendon ruptures are most likely to occur in sports requiring sudden stretching of the tendon, such as sprinting and squash. Occasionally, the Achilles tendon may rupture suddenly from a relatively routine movement like walking down a curb. Achilles tendon ruptures can happen to anyone, but are most likely to occur in people over the age of 40, males more so than females.
An Achilles tendon rupture will require urgent review by a specialist who can help you decide the best course of treatment. This may be surgical repair or conservative management, both of which require a period of immobilisation and then gradual reintroduction of weight bearing and ankle movement. Following this, you will require several months of rehabilitation to help restore your strength and balance and help you return to your normal activities.





